The mRNA Vaccine Revolution: How Science Did the Impossible in Ten Months
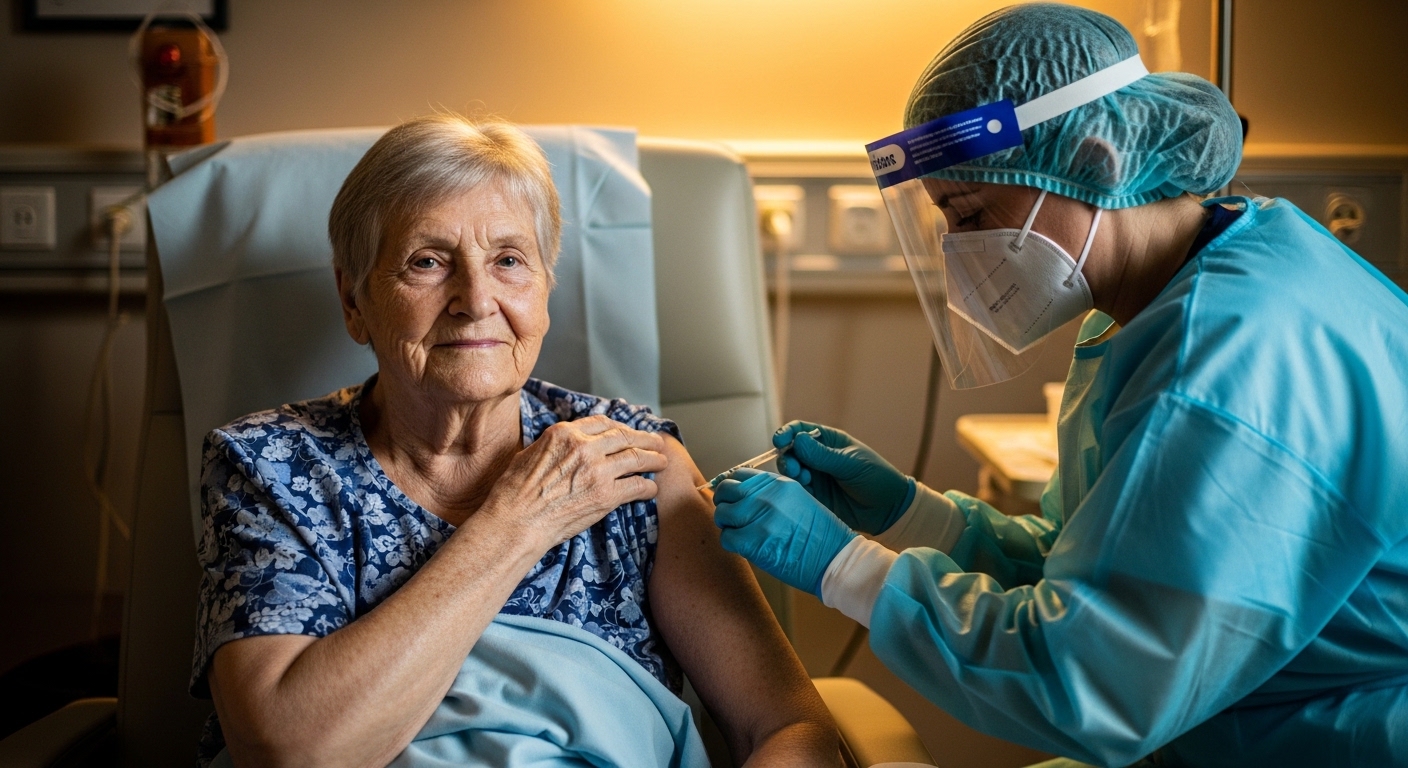
On December 8, 2020, a 90-year-old grandmother named Margaret Keenan became the first person in the world to receive a fully approved COVID-19 vaccine outside of a clinical trial. Sitting in a hospital in Coventry, England, wearing a festive Christmas jumper, she accepted a needle in her arm that represented the culmination of one of the most extraordinary scientific achievements in human history — the development of a safe, highly effective vaccine against a novel pathogen in less than ten months. The normal vaccine development timeline is ten to fifteen years. What happened in 2020 was, by any measure, unprecedented.
The Pfizer-BioNTech and Moderna vaccines that emerged from this effort were not just fast — they were genuinely revolutionary. Both used messenger RNA, or mRNA, a technology that had been in development for decades but had never previously been used in an approved vaccine. The concept is elegant: rather than injecting a weakened or inactivated form of the virus, mRNA vaccines deliver a set of molecular instructions that tell the body’s own cells how to produce a harmless piece of the virus — in this case the spike protein on SARS-CoV-2’s surface. The immune system learns to recognise and attack that protein, and when the real virus arrives, it is met with a primed and ready defence.
The speed was made possible by a combination of factors that are unlikely ever to converge so dramatically again. Decades of prior mRNA research by scientists including Dr. Katalin Karikó and Dr. Drew Weissman — who shared the 2023 Nobel Prize for their foundational work — had solved the key technical problem of making mRNA stable enough to be delivered into human cells without triggering a dangerous immune reaction. The global scientific community, galvanised by the emergency, shared data and infrastructure at an unprecedented pace. Regulatory agencies ran approval processes in parallel rather than in sequence.
The success of mRNA vaccines against COVID-19 has transformed the landscape of vaccine development for all future diseases. Clinical trials are now underway using mRNA technology against HIV, tuberculosis, several cancers, and other infectious diseases for which no effective vaccine previously existed. The speed advantage — once the mRNA sequence for a target protein is known, a vaccine candidate can theoretically be designed in days — means that the next pandemic may face a very different scientific response. Margaret Keenan’s moment was not just a medical milestone. It was the dawn of a new era in human immunology.